July 11, 2013
"Doc, I've got indigestion"
Doc, I’ve got “indigestion”
This is probably one of the more common issues my patients seek my advice for. Unfortunately, “indigestion” means a lot of different things to different people, and it can be, in reality, just a very vague feeling of discomfort in the abdomen, in the mildest of cases.

What is “Indigestion”?
Also called “gastric”, “wind” or “bloatedness”, the symptoms can include any of the following:
- bloating (a feeling of fullness)
- nausea and vomiting
- belching, burping or eructations
- burning sensation in the chest (heartburn)
- acidic sensation in the throat (regurgitation)
- abdominal pain
Medically speaking, these symptoms can loosely be called “dyspepsia”, although the strict definition squares it solely with pain or discomfort around the epigastrium (the central abdominal area just above the umbilicus).
These symptoms may be associated with food intake, either with the amount or the type of food ingested.
What are the causes of “indigestion”?
There are a myriad of causes and can broadly be classified into the following:
Diseases:
- Gastritis and ulcer disease
- Helicobacter pylori infestations or infection
- GORD (Gastro-oesophageal reflux disease)
- Gallstones
- Irritable bowel syndrome
- Stomach cancer
- Gastroparesis (a condition where the stomach is unable to empty completely)
- Pancreatitis
- Thyroid disease
Medications:
- Aspirin and other similar-classed painkillers
- Oral contraceptives
- Steroids
- Certain antibiotics
- Thyroid medication
Lifestyle:
- Smoking
- Excessive alcohol
- Eating too much, too fast, eating high-fat or spicy food, or eating during stressful situations
- Stress and fatigue
What should I do about “indigestion”?
As the symptoms of indigestion are often vague and varied, especially with a wide range of different causes, you should seek a medical opinion from your Family Doctor first. Your Family Doctor will give you a thorough evaluation on your symptoms and complete a physical before deciding what the next course of action should be. Generally speaking, it can be a trial of medication with the appropriate lifestyle changes, or a referral to a Specialist for further evaluation.
If the trial of medications do not help resolve the symptoms, it will certainly be wiser to return to the same Family Doctor, rather than doctor-hop, so that adjustments in the medication, or a specialist referral, can be made.

What further tests can be done to evaluate “indigestion”?
The tests will vary according to your symptoms. Generally-speaking, the typical tests involve endoscopy (gastroscopy with or without a colonoscopy) with either an ultrasound or CT scan of the abdomen.
While endoscopy is an established and safe means of investigations, there are also other alternative tests to evaluate the gastrointestinal tract.

What are the alarming features of “indigestion”?
Most cases of indigestion can be treated successfully by your Family Doctor, but there are certain alarm symptoms and signs that will require a Specialist opinion and possible further tests:
- Weight loss
- Difficulty swallowing
- Recurrent vomiting
- Signs of bleeding (blood, whether fresh or old, in the vomitus or stools)
- Anaemia
- Palpable masses in the abdomen
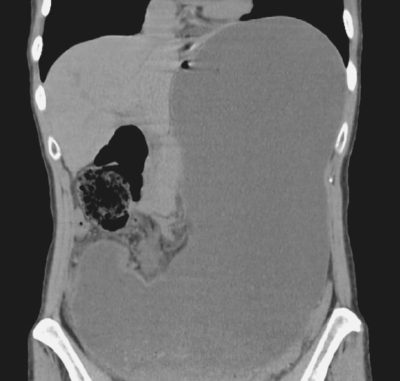
How do I get in touch with a Gastrointestinal Specialist?
To find out more on how you can take steps to further evaluate indigestion and to screen for cancer, please contact Clinic for Digestive Surgery at +65 6570 2702 to speak to SSN Karen, our Clinic Nurse. Alternatively, drop us an email at doctor@clinicfordigestivesurgery.com, or fill up the enquiry form at http://clinicfordigestivesurgery.com/contact and we will attend to your needs at the soonest opportunity.
- Previous article A.M.A. Recognises Obesity as a Disease
- Next article Colorectal Cancer Awareness Month 2013 – Focus on Polyps