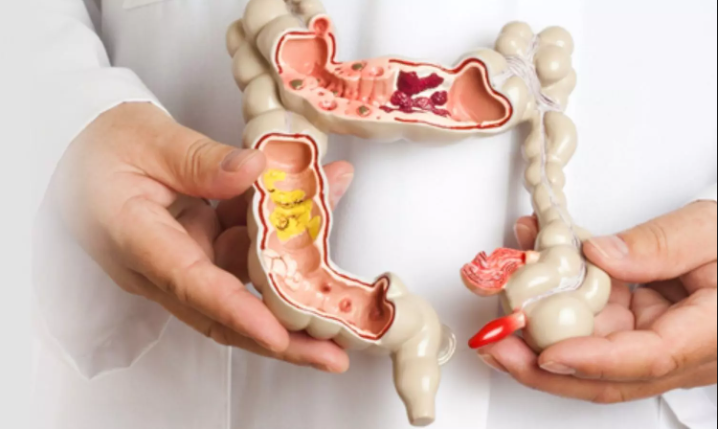
What are Colorectal Conditions?
Colorectal conditions refer to disorders affecting the colon (large intestine) and rectum. These conditions can range from mild to severe and can significantly impact your overall health and quality of life. The colon and rectum play essential roles in the digestive process, including the absorption of water and nutrients and the elimination of waste.
Common Types of Colorectal Conditions
There are several common colorectal conditions, each with its unique characteristics and challenges:
Colorectal Cancer
Colorectal cancer begins in the colon or rectum and can spread to other parts of the body if not detected early. Symptoms may include changes in bowel habits, blood in the stool, abdominal pain, and unexplained weight loss.
Diverticulitis
Diverticulitis occurs when small, bulging pouches (diverticula) in the colon become inflamed or infected. Symptoms include severe abdominal pain, fever, and changes in bowel habits.
Irritable Bowel Syndrome (IBS)
IBS is a functional gastrointestinal disorder characterised by symptoms such as abdominal pain, bloating, and changes in bowel habits (diarrhoea, constipation, or both). It is a chronic condition that requires long-term management.
Inflammatory Bowel Disease (IBD)
IBD includes Crohn’s disease and ulcerative colitis, both of which cause chronic inflammation of the gastrointestinal tract. Symptoms include abdominal pain, diarrhoea, fatigue, and weight loss.
Haemorrhoids
Haemorrhoids are swollen veins in the lower rectum or anus, often causing pain, itching, and rectal bleeding. They can be internal or external and are usually caused by straining during bowel movements or increased pressure during pregnancy.
Anal Fissures
Anal fissures are small tears in the lining of the anus, often resulting from passing hard stools. They can cause pain and bleeding during bowel movements.
Polyps
Polyps are growths on the inner lining of the colon or rectum. While most are benign, some can develop into cancer over time.
Constipation
A condition where the colon muscles do not work properly, leading to severe constipation and difficulty passing stool.
Causes and Risk Factors
Understanding the causes and risk factors for colorectal conditions can help in prevention and management:
- Dietary habits, physical inactivity, and smoking can contribute to the development of colorectal conditions.
- A family history of colorectal cancer, polyps, or other gastrointestinal disorders can increase your risk.
- Conditions such as diabetes, obesity, and chronic inflammatory diseases can elevate the risk of developing colorectal issues.
- The risk of colorectal conditions, particularly colorectal cancer, increases with age, with most cases occurring in individuals over 50.
- A diet high in red and processed meats and low in fibre can contribute to the development of colorectal conditions.
Symptoms
Symptoms of colorectal conditions can vary widely depending on the specific disorder but may include:
- Persistent diarrhoea, constipation, or changes in stool consistency or frequency.
- Pain or discomfort in the lower abdomen is often associated with inflammatory or obstructive conditions.
- Blood in the stool or on toilet paper, which can be a sign of haemorrhoids, fissures, polyps, or cancer.
- Excessive gas and bloating, often associated with IBS or diverticulitis.
- Persistent tiredness and weakness, common in many chronic colorectal conditions.
- Sudden, unintentional weight loss can be a symptom of serious conditions such as colorectal cancer or IBD.
- The presence of mucus in stool, which can indicate inflammation or infection.
Diagnosis
Accurate diagnosis of colorectal conditions is essential for effective treatment. Common diagnostic procedures include:
Colonoscopy
A procedure where a flexible tube with a camera is inserted into the rectum to view the entire colon and rectum. It allows for biopsy and removal of polyps.
Sigmoidoscopy
Similar to a colonoscopy but only examines the rectum and lower colon. It can be used to diagnose conditions in this specific area.
Stool Tests
Tests to detect blood, infections, or inflammation markers in the stool.
Imaging Tests
CT scans, MRIs, and barium enema X-rays help visualise the colon and rectum, identifying structural abnormalities and blockages.
Blood Tests
Used to assess for anaemia, inflammation, and markers of specific conditions like IBD.
Biopsy
A small tissue sample may be taken during a colonoscopy or sigmoidoscopy to check for cancer, inflammation, or other abnormalities.
Treatment Options
Treatment for colorectal conditions varies depending on the specific disorder and its severity. Common treatment options include:
- Anti-inflammatories – Used to reduce inflammation in IBD.
- Antibiotics – For infections causing diverticulitis or other conditions.
- Pain Relievers – To manage discomfort.
- Laxatives and Fiber Supplements – To alleviate constipation in conditions like IBS and constipation.
- Antispasmodics – To reduce cramping and pain in IBS.
- Diet – A balanced diet rich in fiber can help manage symptoms and prevent some colorectal conditions.
- Exercise – Regular physical activity promotes healthy bowel function.
- Hydration – Drinking plenty of water helps prevent constipation.
- Polypectomy – Removal of polyps during a colonoscopy.
- Resection – Removal of part of the colon or rectum affected by cancer, diverticulitis, or severe IBD.
- Hemorrhoidectomy – Surgical removal of haemorrhoids.
- Anal Fissure Surgery – Procedures to promote healing and reduce pain.
- Endoscopic Procedures – Used to treat polyps, bleeding, or other issues without open surgery.
- Laser Therapy – For specific conditions like haemorrhoids.
- Alternative Therapies – Some patients find relief through complementary treatments such as acupuncture, probiotics, and dietary adjustments.
Managing and Preventing Colorectal Conditions
Effective management and prevention strategies can help minimise symptoms and improve quality of life:
- Regular colonoscopies and other screenings can detect colorectal cancer and polyps early, improving treatment outcomes.
- Adopting a balanced diet high in fibre and low in red and processed meats can prevent flare-ups and manage symptoms.
- Techniques such as yoga, meditation, and deep breathing can help manage stress, which can exacerbate GI symptoms.
- Reducing these habits can lower the risk of developing colorectal conditions.
- Adhering to prescribed medications and treatment regimens can effectively manage symptoms and prevent complications.