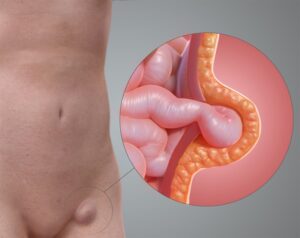
What is Intestinal Perforation?
Intestinal perforation, also known as a perforated bowel, occurs when a hole develops in the wall of the intestine. This condition is a medical emergency because it can lead to the contents of the intestine leaking into the abdominal cavity, causing severe infection and inflammation known as peritonitis. Prompt diagnosis and treatment are crucial to prevent serious complications.
Causes of Intestinal Perforation
Intestinal perforation can result from various causes, including:
Gastrointestinal Disorders
Conditions such as Crohn’s disease, ulcerative colitis, and diverticulitis can weaken the intestinal wall and lead to perforation.
Infections
Severe infections, such as appendicitis, can cause inflammation and rupture of the intestinal wall.
Trauma
Injuries to the abdomen, whether from accidents or surgical procedures, can cause perforation of the intestines.
Foreign Objects
Swallowing sharp objects can puncture the intestinal wall, leading to perforation.
Ulcers
Peptic ulcers in the stomach or small intestine can erode through the wall, causing perforation.
Cancer
Tumours in the intestine can cause obstruction and weaken the intestinal wall, leading to perforation.
Medication Side Effects
Long-term use of certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can increase the risk of perforation by causing ulcers.
Symptoms of Intestinal Perforation
The symptoms of intestinal perforation can vary depending on the location and severity of the perforation but typically include:
- Sudden, intense abdominal pain is a hallmark symptom of intestinal perforation. The pain is often sharp and may spread throughout the abdomen.
- A perforated bowel can lead to infection and inflammation, causing a high fever and chills.
- The leakage of intestinal contents can cause severe nausea and vomiting.
- The abdomen may become swollen and tender to the touch due to the accumulation of fluid and gas.
- Diarrhea, or the inability to pass gas or stool, can occur if the perforation leads to bowel obstruction.
- An increased heart rate may be a sign of infection or internal bleeding.
- Low blood pressure can occur due to blood loss or severe infection, indicating a critical condition.
Diagnosis of Intestinal Perforation
Accurate and timely diagnosis of intestinal perforation is essential for effective treatment. Common diagnostic procedures include:
Physical Examination
A healthcare provider will perform a physical examination, checking for abdominal tenderness, swelling, and signs of infection.
Blood Tests
Blood tests can reveal signs of infection, inflammation, and blood loss, helping to confirm the diagnosis.
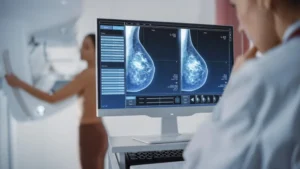
Imaging Tests
- X-rays – Can detect free air in the abdominal cavity, indicating a perforation.
- CT Scans – Provide detailed images of the abdomen, helping to locate the perforation and assess the extent of the damage.
- Ultrasound – Can help visualise fluid accumulation and inflammation in the abdominal cavity.
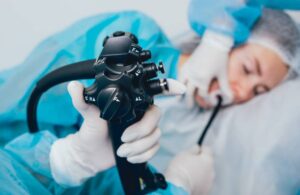
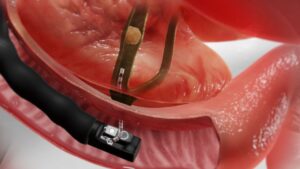
Endoscopy
- In some cases, an endoscopy may be performed to directly visualise the inside of the gastrointestinal tract and identify the source of the perforation.
Treatment Options for Intestinal Perforation
Treatment for intestinal perforation typically involves emergency medical intervention. The main treatment options include:
Surgery
Surgical repair is often necessary to close the perforation and clean the abdominal cavity. The type of surgery depends on the location and cause of the perforation:
- Primary Repair – Directly closing the hole in the intestine.
- Resection – Removing a damaged section of the intestine and reconnecting the healthy ends.
- Colostomy or Ileostomy – In severe cases, an opening in the abdomen is created to divert waste into an external bag.
Antibiotics
Broad-spectrum antibiotics are administered to treat and prevent infection. These medications help control the spread of bacteria and reduce inflammation.
Drainage
If there is an abscess or significant fluid accumulation, drainage procedures may be performed to remove the infected fluid from the abdominal cavity.
Supportive Care
Treatment for intestinal perforation typically involves emergency medical intervention. The main treatment options include:
Complications of Intestinal Perforation
Intestinal perforation can lead to serious complications if not promptly treated, including:
Peritonitis
Inflammation of the abdominal lining due to leakage of intestinal contents. This can cause severe infection and requires immediate treatment.
Sepsis
A life-threatening condition where the body’s response to infection causes widespread inflammation and organ failure.
Abscess Formation
Localised pockets of infection within the abdomen can occur, requiring drainage and antibiotic therapy.
Shock
Severe infection or blood loss can lead to shock, characterised by low blood pressure and organ dysfunction.
Bowel Obstruction
Scar tissue from surgery or inflammation can lead to future bowel obstructions.
Preventing Intestinal Perforation
While not all cases of intestinal perforation can be prevented, certain measures can reduce the risk:
- Proper management of conditions like Crohn’s disease, ulcerative colitis, and diverticulitis can help prevent complications such as perforation.
- Limit the use of NSAIDs and other medications that can cause gastrointestinal ulcers.
- Early treatment of infections like appendicitis can prevent progression to perforation.
- Avoid swallowing foreign objects and practice safe handling of sharp items to prevent accidental injury.
- Regular check-ups with a healthcare provider can help detect and manage potential risk factors early.